Amos Laar, Ph.D. Department of Population, Family and Reproductive Health, School of Public Health, University of Ghana, Accra Ghana. E-mail alaar@ug.edu.gh

Amos Laar, PhD
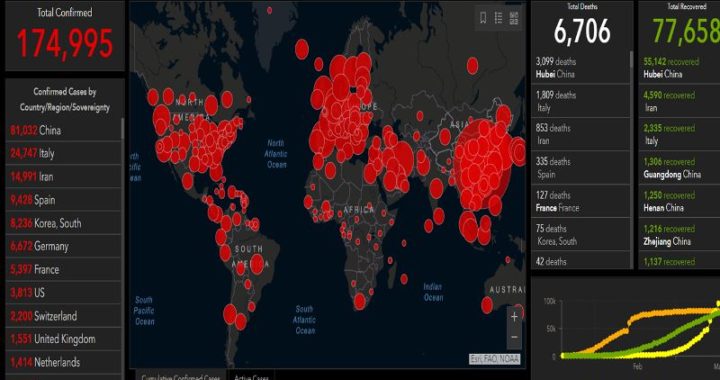
In December 2019, a few cases of a severe form of viral pneumonia were reported from Wuhan city, Hubei Province, China. The illness was identified as a novel Coronavirus – severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2 virus). While investigations are still ongoing, the medical and scientific community believes that this virus may have originated in animals and transmitted to humans at one of several traditional markets in Wuhan. As of midday today – March 16th 2020, over 170,000 have been diagnosed with the disease, which has now been christened COVID-19. At least 6,600 people have died worldwide, and over 77,000 people worldwide have recovered from the disease.
Ghana has instituted several measures in response to COVID-19, which was on March 11th, 2020 officially declared by the World Health Organization (WHO) as a pandemic – an infectious disease that has spread across large regions (e.g., continents) and affected many people worldwide. The measures instituted by Ghana include thermal screening at ports of entry to identify people with fever (or body temperature above 38 degrees centigrade), isolation of the infected, quarantining of the exposed, travel restrictions, and targeted lockdowns (the last two were initiated on March 15, 2020). The Ministry of Health and its service delivery agency – the Ghana Health Service continue to provide health-related prevention guidance – including “sending alert messages to all regions of the country, enhanced screening activities at ports of entry especially the Kotoka International Airport and health facilities”. As of March 15th, 2020, six COVID-19 active cases had been confirmed in Ghana, all of whom are alive. It is probable that several other people in Ghana will be infected by the virus.
So far, about 3% of people with diagnosed COVID-19 have died, while about 5 – 10% require intensive care. That being said, even if a small fraction of the over 30million people in Ghana require care resources like ventilators or extra-corporeal membrane oxygenation to help them breathe, or healthcare providers need personal protective equipment (PPEs) to perform their duties, a difficult triage calculus will be needed. Given this background, is Ghana prepared to respond to pandemics in an ethically sound manner? A paper published by BMC Medical Ethics in 2015, on which I am the lead author, provided an answer. Ghana was not prepared in 2015 and certainly is not in 2020.
We may have failed as a country to plan ethically prior to the declaration of the pandemic, but we have the opportunity to deal with ethics tensions associated with pandemic responses such as quarantining of the exposed, isolation of the infected, social distancing, lockdowns. We are late, but not too late to start talking about how to ethically deal with these tensions. As our distinguished ethicists have warned: “done wrongly, such public health measures can take our rights and freedoms away. But done rightly, they can markedly reduce the spread and mortality associated with this disease”.
For the above, and other reasons, we assessed – in 2015, the ethics-sensitivity of Ghana’s response plan for pandemic influenza. We commended the drafters of the plan on its technical content and fundamental assumptions but criticized the ethics considerations. We noticed that several important ethical issues had been unanticipated, unacknowledged, and unplanned for. These included guidelines on allocation of scarce resources, guidance on healthcare worker duty-to-care, and on compensation; nuanced stockpiling of vaccines/antivirals/PPEs, travel restrictions, and cooperation with neighboring countries. We warned that, until these deficiencies are recognized and addressed, Ghana risks rolling out unjust and ethically indefensible actions with real negative consequences during a pandemic. We requested that inputs be obtained from the public and ethicists during the next revision of the response plan. That was in 2015. So, of what relevance is our recommendations to addressing the enormous challenges being posed to the Ghana health systems by COVID-19? Our recommendations are still very relevant. I justify my answer to the question by highlighting key ethical considerations for pandemic response.
As we discussed in our paper (Laar and DeBruin, 2015), ethical principles to guide preparation before a pandemic, during a pandemic and post-pandemic exist, and may be organized into two broad categories – substantive, and procedural ethics. Substantive ethics principles relate to such concepts as fairness, duty-to-care (especially of healthcare worker), duty-to-steward resources etc. Process-related ethics principles include transparency, consistency, proportionality, accountability, prioritization/allocations of scarce resources, travel restrictions, border control.Pandemic ethics ascribes rights and obligations to both right-holders (individuals) and duty-bearers (governments). The role of governments in protecting, promoting, and assuring the health of their citizenry is grounded primarily in national legislations, but also local policies, and international conventions. Usually backed by state statutes and grounded in scientific evidence, the obligations of governments or public health practitioners are essentially to protect public health. However, such powers (sometimes referred to as the police power) are not absolute in comparison with the interests/rights of the individuals they seek to protect. Outlined in the table below are selected pandemic ethics parameters, with accompanying requirements in pandemic planning and response.
Selected pandemic ethics parameters, with accompanying requirements in pandemic planning and response
| Pandemic ethics parameter | Meaning/requirement in pandemic planning and response |
|---|---|
| Fairness, consistency, and transparency | To be fair, standards of care protocols must be recognized as fair by all affected parties. Treating like groups alike and avoiding invidious discrimination has been suggested as an important way to promote fairness and foster public trust. |
| Decision making process, and justification for delineated actions: | Pandemic preparedness decision-making must be deliberative and all-inclusive, with public consultations. During an pandemic, if public consultations are not possible due to limited time, all actions/activities should be adequately justified |
| Communication to at risk population/information symmetry: | The public should be continuously informed on all aspects of the planned interventions. Communicators should remember that good ethics begin with good facts. |
| Prioritization, and allocation of scarce resources: | Triage systems for priority setting in providing critical care, or for allocation of scarce resources (vaccines, intensive care units, PPEs, hospital beds, human resource allocation, and staffing) during a pandemic should be clearly outlined. Not anticipating, not acknowledging, not putting guidance in place on triaging and prioritization is unfair, inefficient. |
| Healthcare worker duty to care adequately explained: | During disasters, health care professionals’ primary duty is to patients in need of medical care, including when providing care entails some risk to the healthcare provider. Every pandemic response plan should address the rights and responsibilities of healthcare professionals. Given what is known about how COVID-19 spreads, with appropriate precautions, nosocomial transmission can be mitigated. Health care personnel should receive the resources they require as well as training on proper use of the resources e.g. donning and doffing of PPEs, including fit testing of appropriate masks and use of powered air-purifying respirators. |
| Nuanced stockpiling of antiviral, vaccines, PPEs, etc: | Provisions are made for national stockpiling of antivirals, vaccines, and PPEs; and such provisions are sensitive/proportionate to locale-specific competing demands |
| Continuity of essential services: | Efforts are made to ensure continuity of essential services including non-health sector essential services such as ensuring business continuity, capacity for corpse disposal etc. |
| Considerations of equity, social justice, vulnerable groups: | There are deliberate efforts to addresses special needs of vulnerable and disadvantaged groups |
| Social solidarity considerations: | Guidance exists to manage complex social spaces; importance of social “solidarity” during a pandemic is acknowledged and communicated |
| Proportionality of response: | Limitations on services provided should be necessary and commensurate with the scale of the disaster. That is restrictions to individual liberty are carefully thought through and measures taken to protect the public from harm do not exceed what is necessary to address the actual level of risk to, or critical need of, the community. |
| Border issues, travel restrictions, and international solidarity | Pandemic response should explicitly and adequately address international cooperation and solidarity. Closing state or international borders to quell the spread of disease is an option. However, if activated at the wrong time, it may only serve as a political placebo |
While the government indeed has the responsibility to its citizens to respond to COVID-19 and other massive outbreaks in an ethical and medically sound manner, it is in all actuality everyone’s responsibility. The onus cannot only be placed upon the government to control and protect everyone from these infectious disease outbreaks. We as individuals also have the responsibility to keep COVID-19 under control through our own preventative and precautionary actions, herein referred to as “corona etiquette.” Personal corona etiquette are as crucial to controlling this pandemic as governmental action. A few weeks ago, the Ghana Ministry of Health, in its several press releases, enjoined us all to adhere to such measures as:
- Wash hands regularly with soap under running water
- Use alcohol hand rub where available
- Keep a distance of at least one meter from a person showing signs of fever, cough, and difficulty breathing
- Do not touch your eyes, nose, mouth, or face with unwashed hands
- When contact with a sick person or with potentially infected sources or object occurs, avoid touching your eyes, nose or mouth with unwashed hands
- Seek treatment immediately if infection is suspected, if symptoms occur or when advised by a health worker.
- Use handkerchief or tissue paper when coughing and dispose of it responsibly.
- Thoroughly cook meat and eggs and wash vegetables and fruits prior to consumption
- Drink plenty of water, eat well, reduce stress and have enough sleep
Additional responsibilities for travelers who fall sick are:
- Seek medical care right away
- Declare your travel history honestly to your healthcare provider
- Stay at home unless leaving to seek medical attention
- Do not travel while sick
According to what I have seen, read, and heard; it would seem to me that the required efforts to break the chain of transmission are in place. It has been established that the virus spreads rather effectively through person-to-person contact, such as in large social gatherings. With six confirmed cases since last Thursday (March 12th, 2020), Ghanaian residents are in the most critical stage to deny the virus further opportunities to propagate and infect. If Ghana is not able to manage this challenge in the next few weeks, we could have confirmed cases swelling up exponentially, well beyond the carrying capacity of our health system. That is why schools, universities, events and public gatherings have been canceled. Let’s act as responsible denizens – adhering to the precautionary measures outlined by state and global agencies. We should be informed but should not overreact. Let’s exhibit our utmost of personal corona ethics and etiquette – in this challenging time.